Early Detection and Screening for Breast Cancer
Breast Cancer Risk Factors
Remember I talked about being young, thinking that this would not happen to me? Studies have shown that Breast Cancer is caused by a combination of risk factors and being young does not necessarily mean you will not get Breast Cancer. Risk factors increase your chance of getting a disease such as Breast Cancer, but having a risk factor doesn’t necessarily mean that you will get the disease:
Lifestyle-related Breast Cancer risk factors (this means that you can reduce your risk)
- Alcohol Intake
Alcohol has been clearly linked to an increased risk in Breast Cancer with the risk increasing depending on the amount of alcohol consumed. Having 1 alcoholic drink per day gives a small (7-10%) increase in risk compared with non drinkers, while having 2-3 drinks per day increases this risk to about 20% higher than non drinkers for developing Breast Cancer.
- Being overweight or obese after menopause
Before menopause a woman’s ovaries produces oestrogen for the body. After menopause fat cells take over this role, therefore women who are overweight after menopause will have more fat cells to produce more oestrogen thus increasing your risk of Breast Cancer.
- Physical inactivity
There is increasing evidence that proves that physical inactivity can increase Breast Cancer risk especially after menopause. According to the World Health Organisation (WHO) adults aged 18-64 should have at least 150 minutes of moderate-intense aerobic physical activity or at least 75 minutes of vigorous-intensity aerobic physical activity throughout the week.
- Reproductive history
Women who have their first pregnancy after the age of 30, or do not breastfeed have a slightly higher breast cancer risk overall. Having multiple pregnancies and becoming pregnant at an early age reduces Breast Cancer risk.
- Birth control
Oral contraceptive pills: Most studies have linked oral contraceptive users with a higher risk of breast cancer compared to non-users. However, this risk goes back to normal after 10 years.
Birth control injections: Depo-provera is an injectable form of progesterone that is administered every 3 months for birth control. Some studies have linked this type of birth control with an increased risk of Breast Cancer but some have not.
Birth control implants, Intrauterine devices (IUDs), skin patches, vaginal rings: As these types of birth control use hormones they could theoretically influence Breast Cancer growth. This link has been studied more in hormone-releasing IUDs but less on implants, patches and rings.
- Hormone Replacement Therapy (HRT)
There are 2 main types of HRT to control symptoms menopause in women: Combined HRT which have both oestrogen and progesterone and Estrogen-only therapy. The use of combined HRT after menopause has been linked to increased Breast Cancer risk. This risk is typically seen after 4 years of use with the risk decreasing after 5 years of stopping HRT. Regular monitoring during treatment should also be done.
Breast cancer risk factors that cannot be changed
- Getting Older
The risk of Breast Cancer increases with age; most new diagnosis of Breast Cancer occurs after age 50 but still significantly rises after age 40. Hence, the emphasis on getting a screening mammogram once you hit 40 years old. Our Singapore government has been very active in this area and do allow us to dip into our Medisave accounts or utilise their Screen for Life programmes.
- Genetic Mutations
About 5% to 10% of Breast Cancers are thought to be linked to hereditary gene changes (mutations) which are passed on from a parent. The most common cause for hereditary Breast Cancer is an inherited mutation in the BRCA1 or BRCA2 gene. (Think of Angelina Jolie here). Normally these genes are involved in repair of damaged DNA but mutated versions of these genes lead to abnormal cell growth, which can lead to Cancer.
On average, a woman (or man) with a BRCA1 or BRCA2 gene mutation:
a) has a 7 in 10 chance of getting Breast Cancer by age 80;
b) is more likely to be diagnosed with Breast Cancer at a younger age; and
c) has higher risk of developing Ovarian Cancer and certain other types of Cancers.
- Having a family history of Breast Cancer
Overall, about 15% of women with breast cancer have a family history of the disease. Having a first-degree relative (mother, sister or daughter) with Breast Cancer almost doubles a women’s risk. Having 2 first-degree relatives increases the risk further by about 3 folds.
- Age of menarche and menopause
Having early onset of menstrual periods before age 12 and menopause after age 55 expose women to hormones for longer, theoretically raising their risk of breast cancer.
- Having dense breasts
Breasts that are dense have more connective tissue then fatty tissue which can sometimes make it hard to see tumours on a mammogram. Women with dense breasts on mammogram had a 1 ½ to 2 times increased risk of breast cancer compared to a woman with average breast density.

Diagnosis is the start of a long journey
I cannot overemphasise on the strong support that is required. My pillars of support would definitely be my husband first and foremost, followed by my mother, the rest of my family and the amazing support I got from my friends. My husband has walked beside me every single step of the way, giving me strength when I had none. He lovingly said to me: “I am with you always, the only place I cannot be with you is in your dreams”. Hence, when I was going through this dark period of nightmares and insomnia, I would wake him up and he would comfort me.
COVID-19 complicated my family’s situation as they resided in Malaysia and Brunei and were unable to fly in immediately to be with me during the initial diagnosis. We had to get special permission for them to fly in on compassionate reasons. COVID-19 strengthened my family bonds and I am so grateful that they endured the swabbing and quarantine on my behalf. I have always been very close to my family and having them with me was an integral part of my healing process.
I am also very thankful to my business partner Dr Wenus for shouldering the burden of managing the centre when I was away for about six months undergoing my treatment. Being blessed with such strong support, I remained positive and was able to return back to a new version of my normal life. I hope through my experience I am able to help others by stressing on the importance of early detection and providing support for other cancer patients.

Young and Planning for a Second baby
I am Dr Juliana Latif, the co-founder of Fusion Medical, which is a one-stop health screening practice located at Wheelock Place (Orchard).
I delivered my firstborn son at the age of 37 years old and put myself through 1 year of breastfeeding. The second month after stopping breastfeeding, my husband and I decided to continue with our family planning and scheduled our IVF procedure for our second child.
Little did I expect that my regular Breast Self Examination (BSE) done once a month would save my life. I detected a lump in my left breast when I was still breastfeeding my son. I thought it was just a blocked milk duct. Afterall, I was below the age of 40. An ultrasound check on this lump just a week before the scheduled IVF procedure turned my world upside down.
Book your breast cancer screening now!
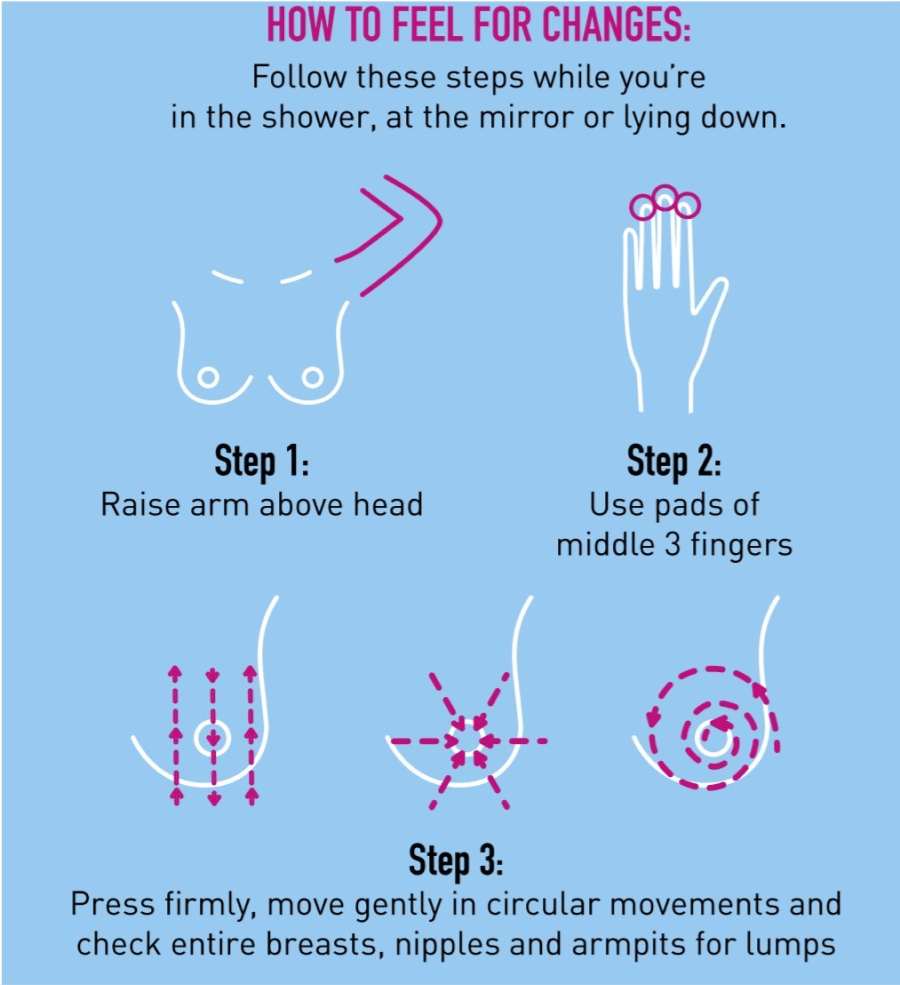
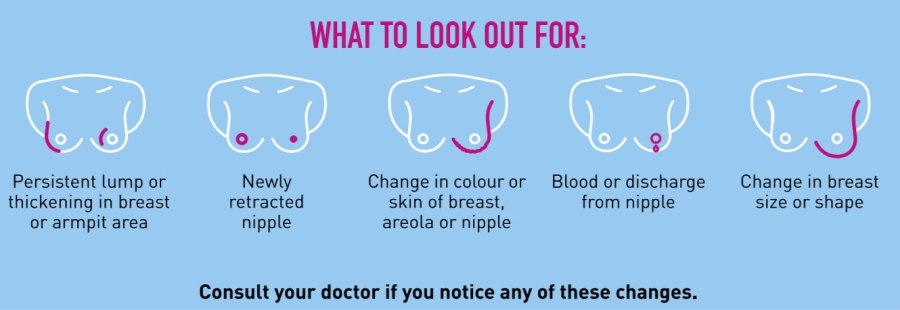
Breast Self Examination (BSE)
When should one start?
The Singapore Cancer Society recommends that women as young as age 20 can start doing monthly self-breast examinations.
BSE should be timed on a monthly basis 7-10 days from the start of your menstruation. If you have stopped menstruating, you can do your BSE on the same date each month.
*The images above were extracted from the Breast Cancer Foundation (Singapore). The full PDF file on breast self-examination can be found in the following link.
What happens when I detect a lump?
Additional checks would be advised upon discovery of a lump. These typically include breast ultrasound and /or mammography. You may wish to consider upgrading your mammography to that of a 3-dimensional one if you have a history of dense breasts.
Lumps that look suspicious on imaging will then require a biopsy to determine the nature of the cells. The good news is majority of breast biopsies do not turn out to be breast cancer. Follow up and treatment may still be recommended by the doctor to manage the benign lesion.
If cancer cells are found, a detailed report will be provided to determine the next steps in management. These include the tumour type and the tumour’s growth rate or grade.
What is important to note is to seek medical attention early. I was lucky that even though I ignored my breast lump initially, I was able to detect it early for the appropriate treatment to be administered. It was most heart-wrenching to kiss my one-year old son goodbye before tearing myself away from him for my PET/CT scan appointment to check if my cancer had spread. The two-hour long procedure was the longest journey of my life before I got informed that my cancer was localised.
Does discovery of a lump mean Breast Cancer?
My breast lump turned out to be invasive carcinoma.
However, you may be comforted and surprised to know that there are more benign (non-cancerous) breast conditions than cancerous ones:
a) Non-proliferative lesions: The most common being breast cysts and the increase in breast cancer risk is very small.
b) Proliferative lesions without atypia (cell abnormalities): These lesions have excessive growth or cells in the ducts or lobules of the breast but do not look very abnormal. They include ductal hyperplasia (without atypia), fibroadenoma and sclerosing adenosis.
c) Proliferative lesions with atypia: In these conditions, the cells in the ducts or lobules of the breast tissue grow excessively, and some of them no longer look normal. These types of lesions include ductal hyperplasia, atypical lobular hyperplasia and intraductal papillomas. Breast cancer risk is about 4 to 5 times higher than normal in women with these changes.
Nevertheless, despite the fact that these conditions are non-cancerous, having them can increase your risk of eventually developing Breast Cancer. Thus, it is important that you monitor these conditions on a regular basis, usually between 3 months to one year depending on what your doctor advises.
Screening of Breast Cancer
Mammogram
A mammogram is a low dose X-ray picture of the breast. It can detect the presence of cancerous lumps even before they can be felt with the hand. Screening mammograms are routinely used to screen for breast cancer in women who have no specific symptoms. Diagnostic mammograms are done after a suspicious results, abnormal physical finding or screening mammogram. The diagnostic mammogram is to determine if these suspicious or abnormal findings are indicative of breast cancer. Compared to screening mammogram, diagnostic mammograms are more detailed .
What is digital breast tomosynthesis?
Digital breast tomosynthesis (DBT) is 3D mammography that allows the breast to be examined 1 layer at a time instead of 1 flat image. DBT may be used together with 2D digital mammography as an additional tool in screening. To the patient, the DBT experience is very similar to a 2D mammography and the X-ray dose remains very low and under the guidelines of FDA. To the radiologist who is the specialist reading the images, the DBT provides additional views of the breast to better analyse the breast tissue.
Ultrasound
A breast ultrasound is a scan that uses sound waves. The breast tissue deflects these waves causing echoes, which provide a picture of the breast tissue. It has the ability to differentiate between a mass that is filled with liquid from a solid mass. Ultrasounds are helpful when a lump is felt, and the images can be used to further evaluate the abnormality. It also helps to measure the exact size and location of the lump and analyse the surrounding tissue.
MRI
If initial diagnostic imaging is inconclusive, a breast MRI (magnetic resonance imaging) may be recommended. MRI uses magnetic energy and radio waves (not radiation) through the breast tissue to create a detailed picture which allows to distinguish between normal and diseased tissue.
Visit Us
Start your skin health restoration journey with us today!
Fusion Medical @ Wheelock
Mon-Fri :8:30am – 5:30pm
Sat :8:30am – 1:00pm
Sun / PH :Closed
Fusion Medical @ Fusionopolis
@ One-North , Singapore 138542
Mon-Fri :8:30am – 5:30pm
Sat/Sun / PH :Closed
About Fusion Medical
Fusion Medical was set up in the year 2015. Our founders, being passionate about offering one-stop quality healthcare services at affordable rates, decided to set up an Executive Medical Centre equipped with diagnostic and imaging equipment under one roof to provide convenience to our patients. Diagnostic and imaging equipment include X-Ray, Ultrasound, Treadmill, Echocardiogram, Tonometry, Mammogram, Retinopathy and Bone Densitometry.
Why Choose Fusion Medical
We Make Things Easy For You
Our clinic is centrally located in Wheelock Place, giving you easy access to quality healthcare services whenever you need it. Appointments are easy, too. Request an appointment online or call us.
Female Doctors Who Understand You
Our female doctors offer a broad range of screening and medical services, personalised just for you. Doctor-patient relationships can last a lifetime, and we believe that it is important to have a doctor who truly understands you. We strive to do the best we can to make you feel comfortable.
Fully Equipped Clinic
We are committed to meeting your specific needs at our clinic. Our clinic is fully equipped with diagnostic and imaging equipment to provide one-stop convenience for you.
Visit Us
Start your skin health restoration journey with us today!
Fusion Medical @ Wheelock
Mon-Fri :8:30am – 5:30pm
Sat :8:30am – 1:00pm
Sun / PH :Closed
Fusion Medical @ Fusionopolis
@ One-North , Singapore 138542
Mon-Fri :8:30am – 5:30pm
Sat/Sun / PH :Closed